Save Time… Save Money… Save Lives…!
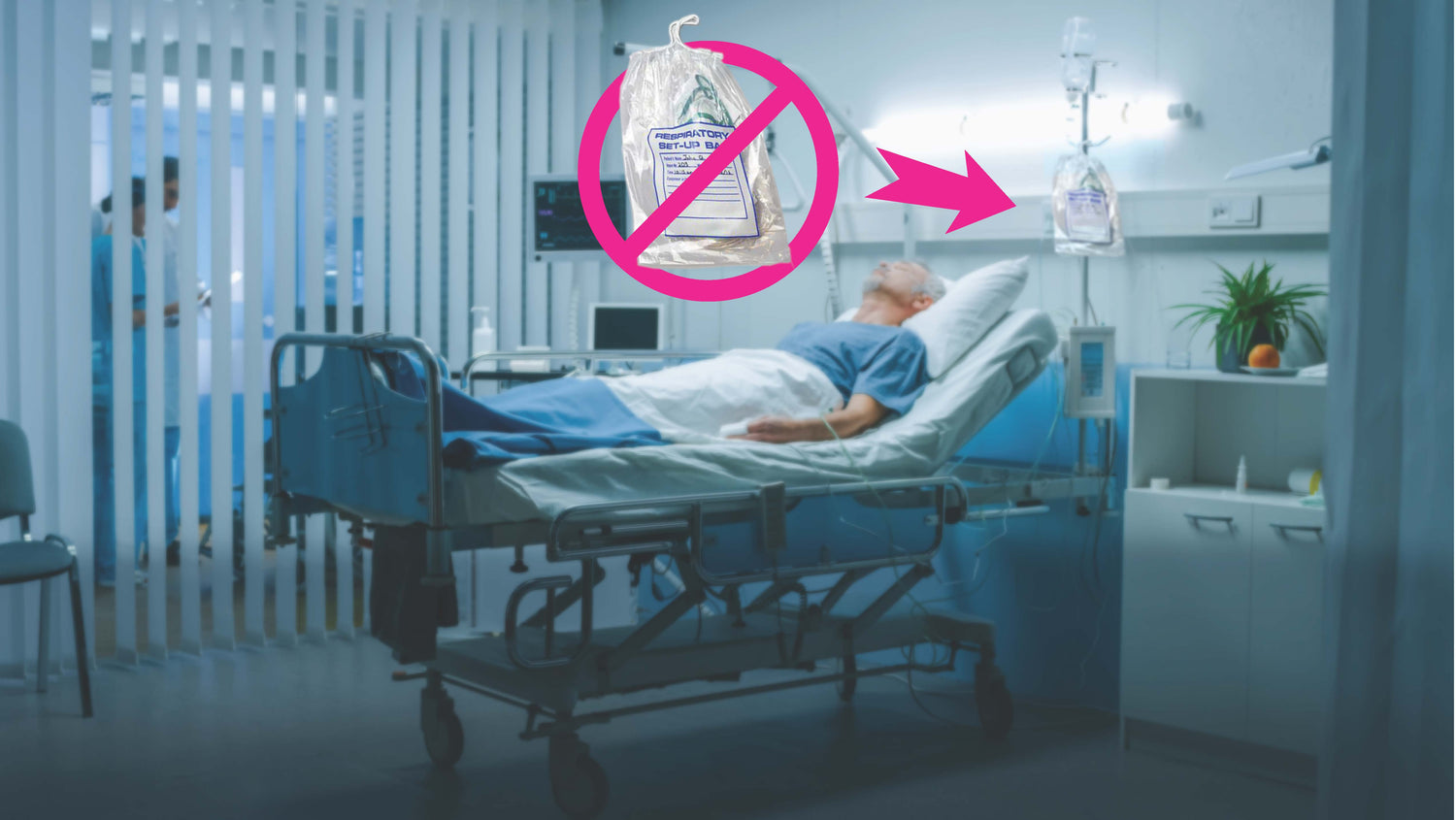
WikiPouch® creates safe, economical, sustainable healthcare products that reduce healthcare acquired infections (HAI) when used for storing reusable patient care items compared to Plastic Bags.
Protect Yourself, Patients & Staff with WikiPouch® Family of Products

Make the switch to WikiPouch®. A Breathable Moisture Wicking Pouch
Shop Our Products